MSHS welcomes Implementation Science Prof Jill Francis back to Melbourne
It was no mean feat for Professor Jill Francis to relocate from the UK during the uncertain times of COVID-19. But after countless cancelled flights and more quarantines than she had imagined, we are delighted to welcome her to the School of Health Sciences as Professor of Implementation Science to develop her broad interdisciplinary research across the Faculty.
 Implementation science investigates methods to improve the adoption and integration of evidence-based practices, policies and interventions into health care. It aims to improve the speed and effectiveness of translating health knowledge into practice, and Prof Francis is determined to see it happen through her work.
Implementation science investigates methods to improve the adoption and integration of evidence-based practices, policies and interventions into health care. It aims to improve the speed and effectiveness of translating health knowledge into practice, and Prof Francis is determined to see it happen through her work.
“Despite all the fantastic training, skill and dedication of staff, hospitals, social care and aged care often fall short of the evidence-based standards they’d like to see,” says Prof Francis, identifying the global issue at stake.
“Inappropriate variations in care drive inequalities of health outcomes, and that’s one of the problems that implementation science addresses”.
It’s a hot topic for many reasons, but primarily for its effectiveness in boosting efficiency of health care systems, a bi-product of which is reducing unnecessary economic strains.
Prof Francis has been involved in a range of implementation science projects throughout her career, both overseas and within Australia, including trying to drive down antimicrobial resistance by reducing overuse of antibiotics, and addressing the overuse of blood transfusions in hospitals.
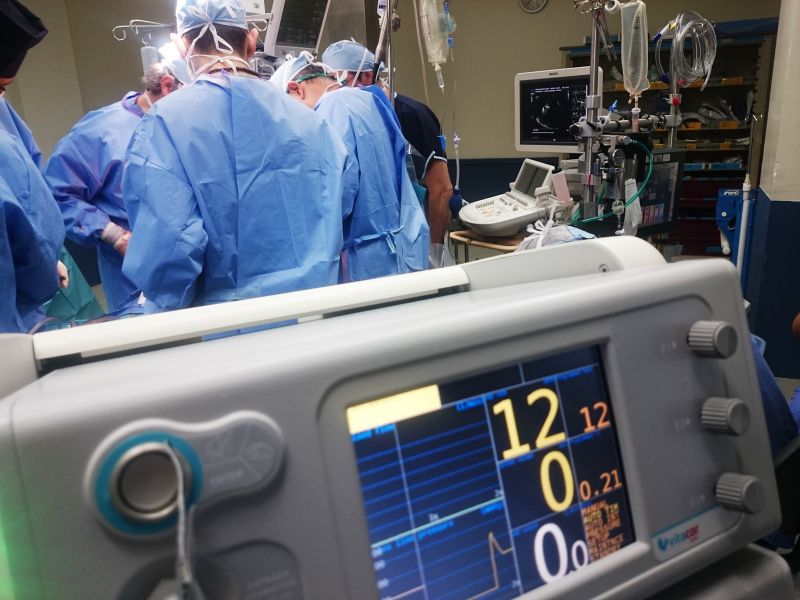
“The average time to adopt a new clinical intervention is 17 years, and established practices can take a long time to supersede. An example is the overprescribing of antibiotics, despite resistance and overuse being observed over half a century ago.”
“Implementation research is discovery research,” she says. “We don’t already know the answers, but we do know the robust research methods that we need to deliver them.”
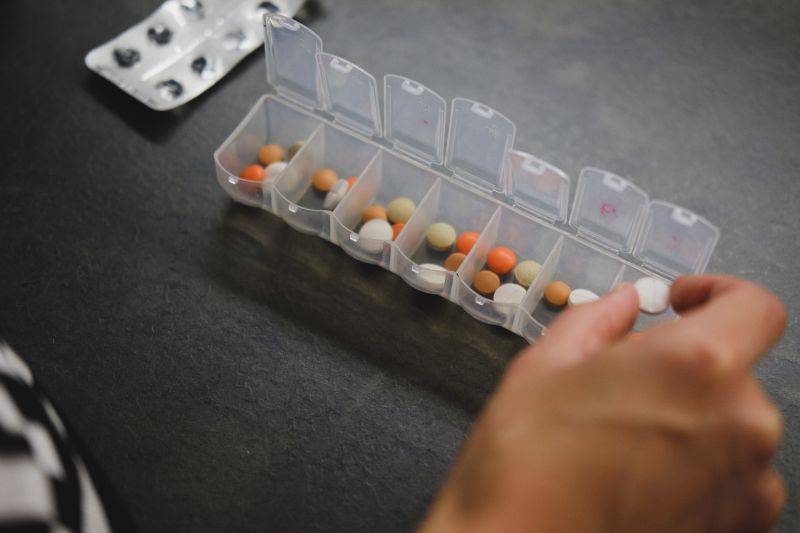
Overseas, Prof Francis investigated appropriate polypharmacy prescribing for older patients (with Queen’s University Belfast), and solution-focused therapy for people with psychosis to improve quality of life (in low and middle income countries in Southeast Europe, with Queen Mary University of London).
When healthcare organisations choose their quality improvement strategies, it is tempting to use popular anecdotal evidence in favour of empirical evidence, but Prof Francis believes implementation science can provide solid evidence to support these activities and increase the likelihood that they’ll be effective.
“Just as randomised controlled trials are regarded as the gold standard for testing clinical interventions, these designs and methods are increasingly being used to find out what works, and how to support clinical practice change”.
Prof Francis has a strong connection to the University of Melbourne and MDHS. Specialising in behaviour change, she received her PhD in social psychology from UoM in 1998. It’s a theme that has continued to underpin and influence her research.
“Using empirical studies to test and refine theories of behaviour gave me a keen sense of skepticism, especially in regard to the many unconscious biases people have about their own behaviour, and the idea that people don’t have great insight into the causes of their behaviour,” she says.
“We need to be cautious about measurement strategies and the attributions people make about why they do what they do”.

For Prof Francis, COVID-19 is an interesting example of how new clinical practices and healthy behaviours can be taken up quickly and effectively under pressure. She is encouraged by her observation that behaviour change can occur extremely rapidly when the priorities of mass media, governments and the general public are aligned. But most importantly, that these changes support and are informed by science.
Slow uptake of best practice is an ongoing problem in all health systems worldwide. Prof Francis aims to address this problem via implementation science research, leading to the faster and more effective uptake of new treatments and research. She is delighted to be in Australia and joining the UoM MSHS team, even if most of her first meet and greets are on Zoom.
“It has taken me a while to get here during COVID, but I’m glad to be here and jump into this opportunity, which provides me with the chance to do lots of interesting research with teams of great people. My strategy is to build a team of implementation researchers who can collaborate across the whole faculty.”
An exciting ‘research exchange’ online event was held on 15 September, where researchers from the Schools of Health Science and Population and Global Health met to talk about their work. Over 100 staff attended and about 30 people gave short presentations.
“The follow-up emails have been exciting. Even using the Webinar mode, this was a great way to connect with other researchers and explore how we could work together in new ways,” explains Prof Francis.
“MDHS is the most amazing powerhouse for research integrity and quality. The possibilities seem endless. I’m looking forward to discovering what we can do together.”